Glaucoma is a common eye condition that affects the optic nerve and most often occurs in older adults. In its early stages, there are virtually no symptoms. It develops slowly and silently, gradually affecting side (peripheral) vision before central vision becomes impaired. The good news is, with timely diagnosis and treatment, many patients can preserve their sight and maintain a good quality of life.
What is Glaucoma?
Glaucoma is a group of eye conditions that gradually damage the optic nerve, the vital connection that sends visual signals from your eyes to your brain. This damage is often linked to increased pressure inside the eye (intraocular pressure), though in some people, it can occur even when the pressure is within the normal range.
Because glaucoma usually develops slowly and without pain, many people do not realise they have it until vision loss has already occurred. Once damaged, the optic nerve cannot be repaired, which is why early detection, regular and consistent management are essential.
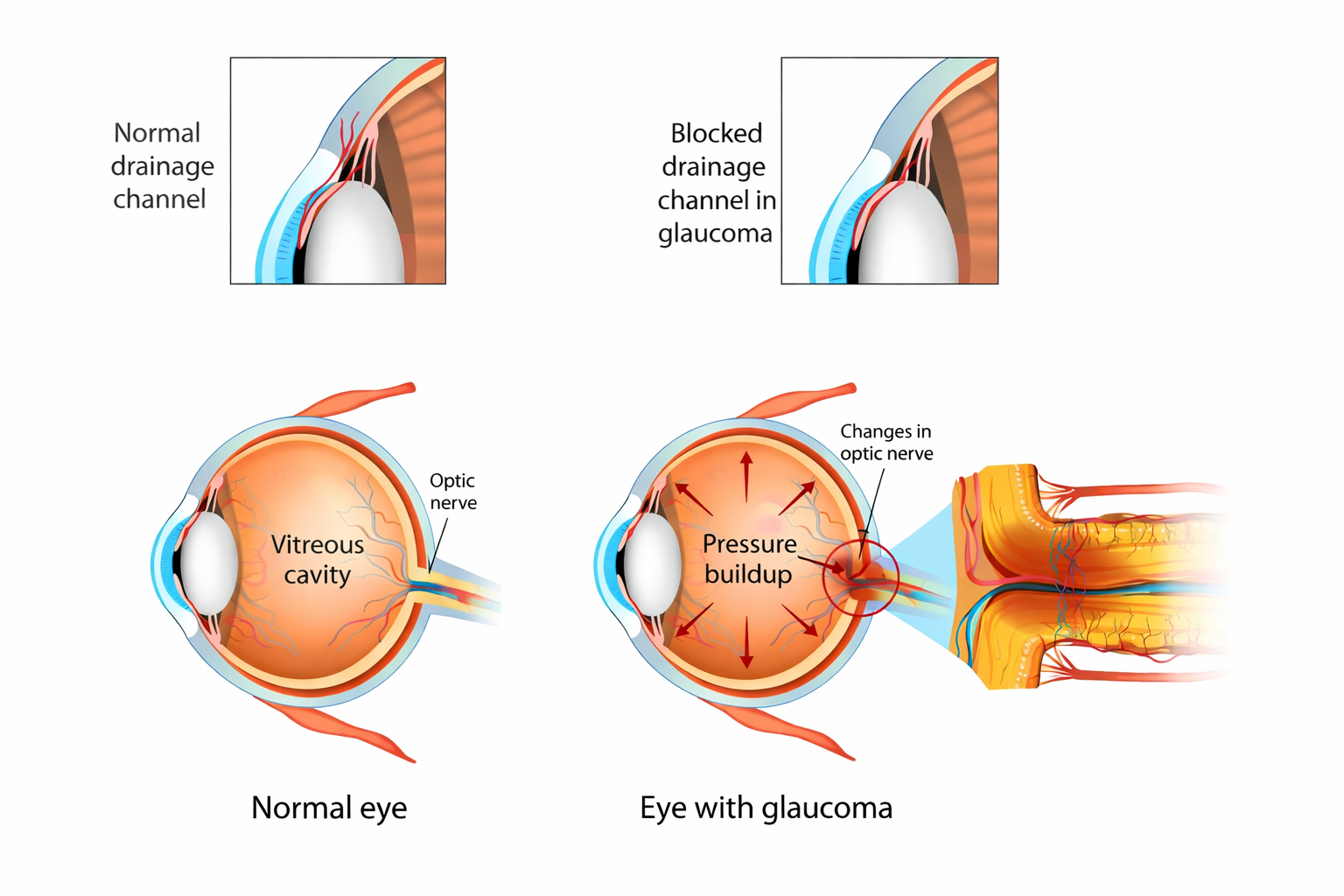
The good news is that with timely diagnosis and proper treatment, glaucoma can be effectively controlled. By keeping eye pressure within a safe range and monitoring changes closely, many patients can preserve clear and stable vision for years to come.
What are the Symptoms of Glaucoma?
In its early stages, glaucoma often causes no symptoms, earning it the nickname “the silent thief of sight.” The condition usually begins by affecting side (peripheral) vision, so changes are subtle and easy to miss.
As glaucoma progresses, you may notice:
- Gradual loss of peripheral vision
- Blurred or hazy vision
- Difficulty seeing in dim light or at night
- Eye discomfort or pressure

Normal Vision

Loss of Peripheral Vision
Normal Vision
Loss of Peripheral Vision
Because these signs typically appear only after significant nerve damage has occurred, regular eye examinations are the best way to detect glaucoma early, before it affects your vision.
Angle closure is the precursor to development of full fledged angle closure glaucoma. This condition is caused by a naturally narrower drainage angle in the eye, where blockage of the outflow by a bulging iris more easily occurs. Specific symptoms of angle closure include:
- Pain or discomfort around the eyes, especially when going from a brighter to darker environment
- Headache or brow ache
- Eye redness
- Blurry vision
- Rainbow coloured rings around lights
If you experience sudden eye pain, headache, nausea, or blurred vision, seek medical attention immediately, as these may indicate acute angle closure glaucoma, a condition that requires prompt treatment.
Who is at Risk?
Anyone can develop glaucoma, but the risk is higher if you:
- Are over 40 years old
- Have a family history of glaucoma
- Have elevated eye pressure
- Live with medical conditions such as high blood pressure, heart disease or obstructive sleep apnoea.
- Have high myopia
- Have narrow drainage angles in the eye (due to a naturally smaller eye, or a family history of narrow angles)
- Use long-term steroid medications (e.g., oral medications, nasal sprays, inhalers, eczema creams, or eyedrops)
- Have had previous eye injuries
Because glaucoma can progress without symptoms, those with these risk factors should schedule regular eye check-ups to detect glaucoma early and protect their vision.
What are the Types of Glaucoma?
Glaucoma is classified into several types, each defined by how fluid drains from the eye and how the optic nerve is affected. Knowing the type of glaucoma you have, helps your doctor choose the most effective treatment to protect your vision.
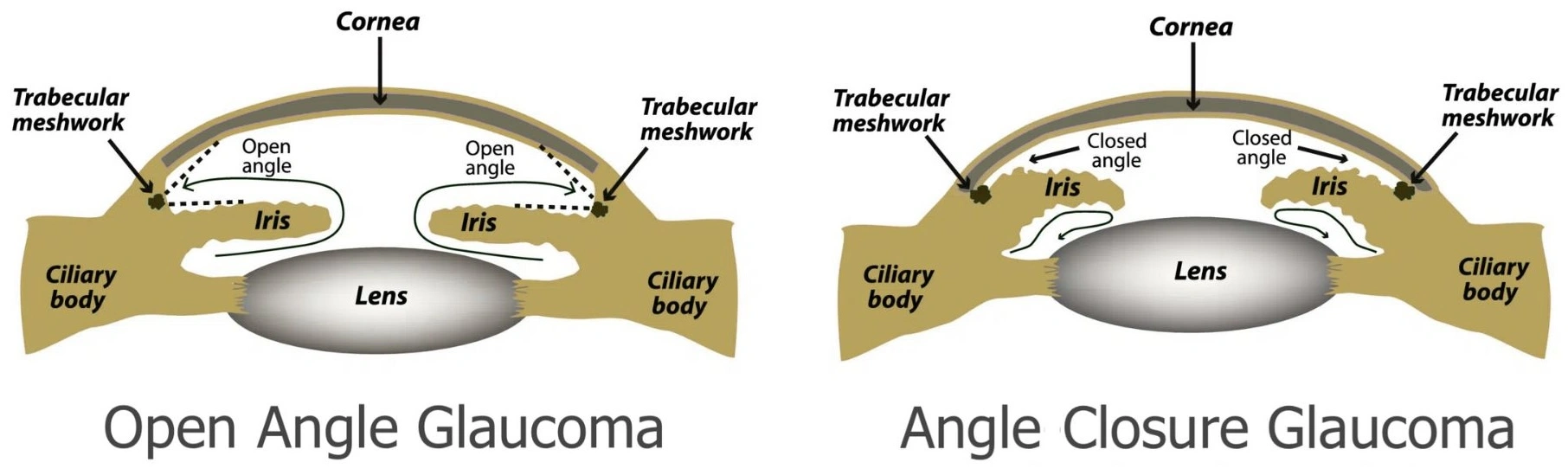
- Open Angle Glaucoma – The most common form, developing gradually as drainage channels become less efficient over time, causing pressure to build up over time.
- Angle Closure Glaucoma – A type of glaucoma where the drainage angle suddenly (acute form) or gradually (chronic form) becomes blocked by the iris, leading to a rise in eye pressure.
- Normal Tension Glaucoma – Damage to the optic nerve can occur even when eye pressure is within the normal range.
- Secondary Glaucoma – Caused by other eye problems such as inflammation, trauma, or prolonged use of certain medications.
Each type of glaucoma requires a different management plan. Regular eye examinations and precise diagnosis are key to detecting changes early and preserving vision for the long term.
How is Glaucoma Diagnosed & Monitored?
Glaucoma is diagnosed through a comprehensive eye examination, as it often develops without noticeable symptoms in the early stages. Assessment typically includes measuring eye pressure, examining the optic nerve, checking visual fields, and evaluating the drainage angle of the eye. Imaging tests may also be used to document the structure of the optic nerve.
Once diagnosed, glaucoma requires regular monitoring. Follow-up visits help track changes in eye pressure, optic nerve health, and visual field results over time. This ongoing monitoring allows treatment to be adjusted when needed, with the aim of slowing disease progression and preserving vision.
What are the Treatment Options?
- Medications as the First Step In the early stages, prescription eye drops or tablets may be prescribed to lower eye pressure, either by improving fluid drainage or decreasing fluid production. At Ascend Eye Clinic, we prioritise optimal treatment using medications with maximal pressure-lowering efficacy and the least profile of medication-related side effects. We use preservative-free glaucoma eye drops to minimise these side effects, and newer agents for patients who have not responded to conventional medications.
- Laser Treatments: Gentle and Effective
Minimally invasive laser procedures help improve fluid flow and control pressure with little downtime.
Several types of laser treatments are available, depending on the type of glaucoma:
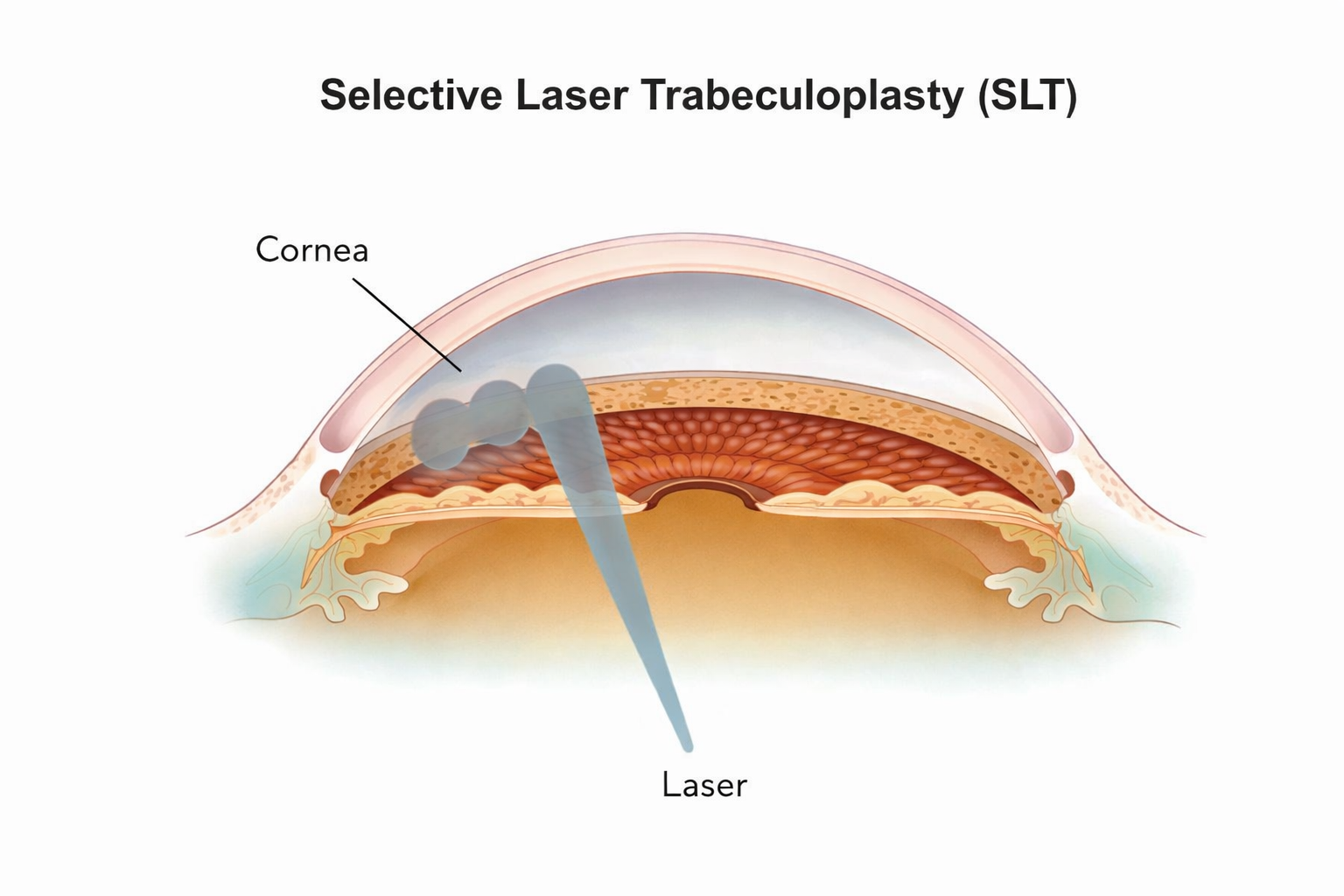
- Selective Laser Trabeculoplasty (SLT): Enhances drainage in open angle glaucoma, allowing reduction or cessation of glaucoma medication usage. This procedure can be repeated for enhanced efficacy.
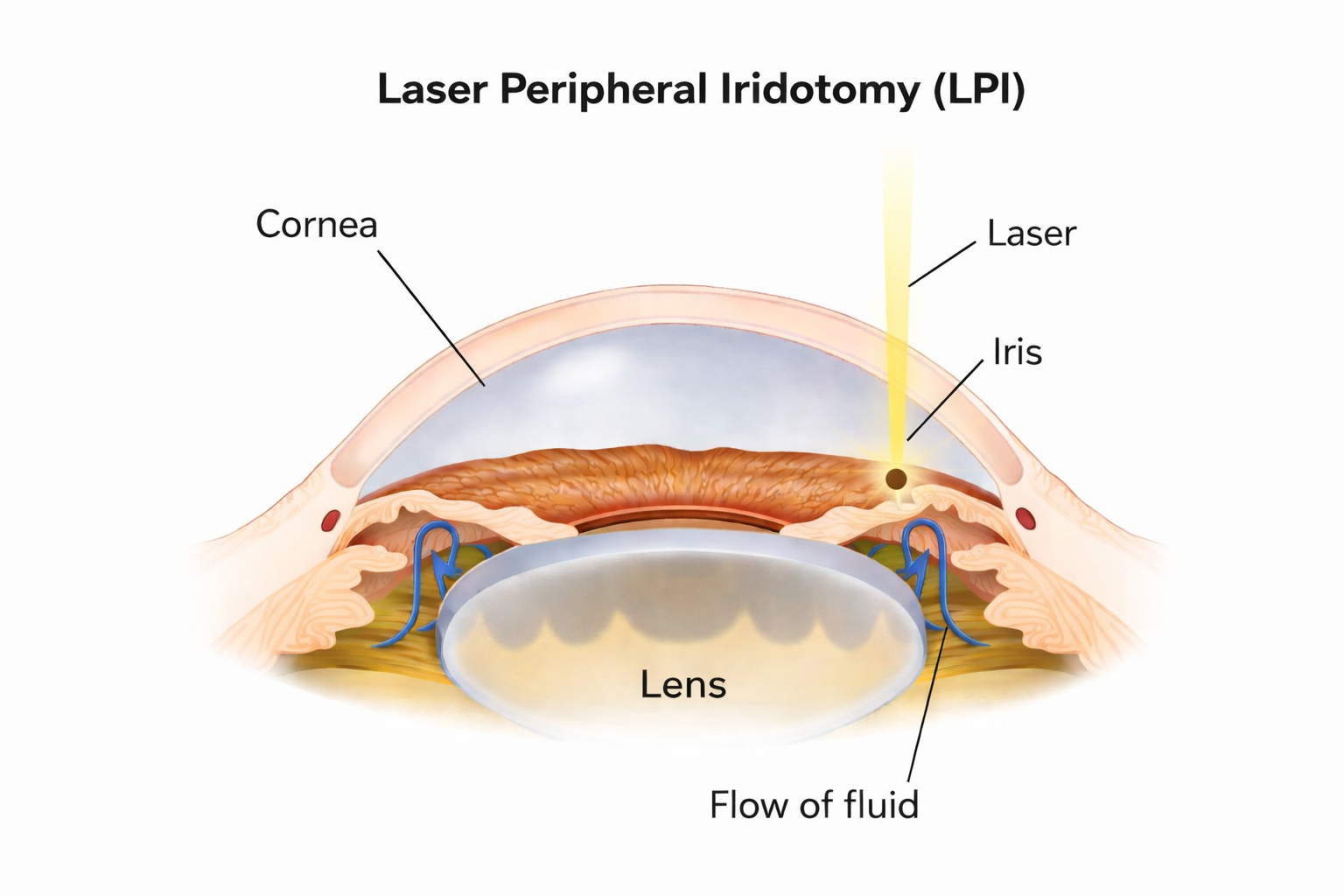
- Laser Peripheral Iridotomy (LPI): A small opening is created in the iris to help fluid move freely and relieve pressure for angle closure glaucoma.
- Micropulse Laser: A novel technique using gentle pulses to improve fluid drainage with minimal impact on eye tissues.
- Diode Laser: For advanced primary or secondary glaucoma cases, one or more treatments of diode laser is effective in lowering eye pressures to lower levels.
- Selective Laser Trabeculoplasty (SLT): Enhances drainage in open angle glaucoma, allowing reduction or cessation of glaucoma medication usage. This procedure can be repeated for enhanced efficacy.
- Minimally Invasive Glaucoma Surgery (MIGS)
For patients with mild to moderate glaucoma who require lowering of eye pressure, Minimally Invasive Glaucoma Surgery (MIGS) is effective in achieving this outcome. These modern procedures use tiny incisions and microscopic devices to improve the eye’s natural fluid drainage, allowing quicker recovery and less discomfort. Common options include:
- Glaukos iStent inject W: Tiny titanium stents placed inside the eye’s drainage system to help fluid flow naturally.
- Hydrus Microstent: A flexible device inserted into the drainage canal to open it and lower pressure.
- Conventional Glaucoma Surgery: For Advanced Glaucoma
When medications, laser therapy, or minimally invasive procedures are no longer sufficient, conventional glaucoma surgery such as trabeculectomy or glaucoma drainage implants is recommended to create new drainage pathways and protect the optic nerve from further damage. Two main types include:
- Trabeculectomy: A surgical technique that creates a tiny channel in the wall of the eye to allow fluid to drain externally and to be carried away by the blood circulation.
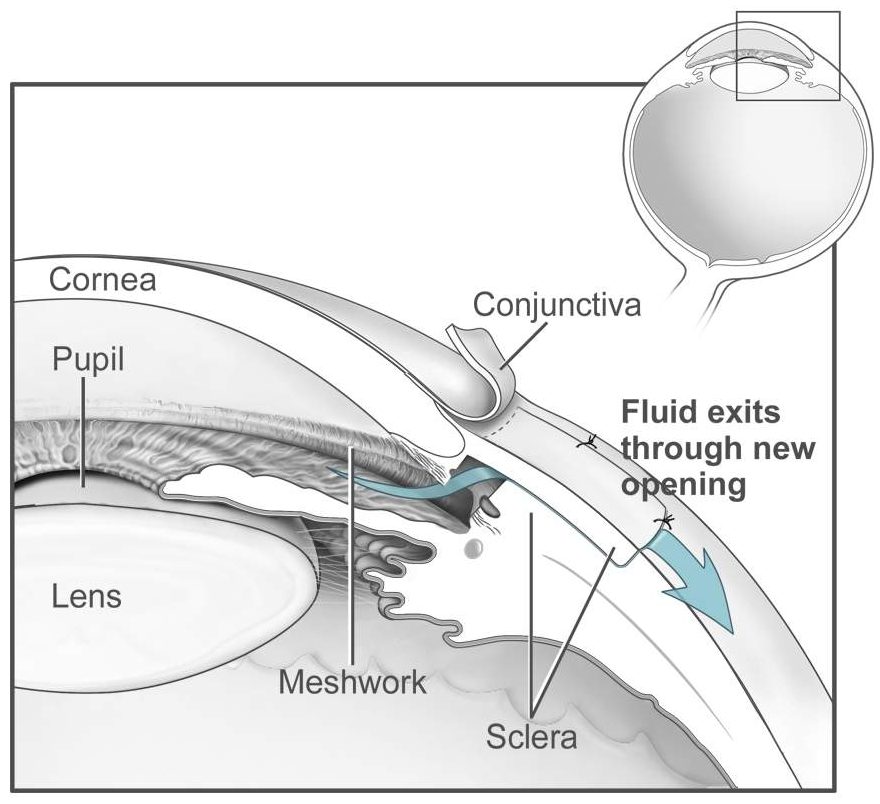
-
- Glaucoma Implants (Drainage Devices): Fine medical grade silicone tubes that are inserted into the front chamber of the eye to facilitate fluid drainage.
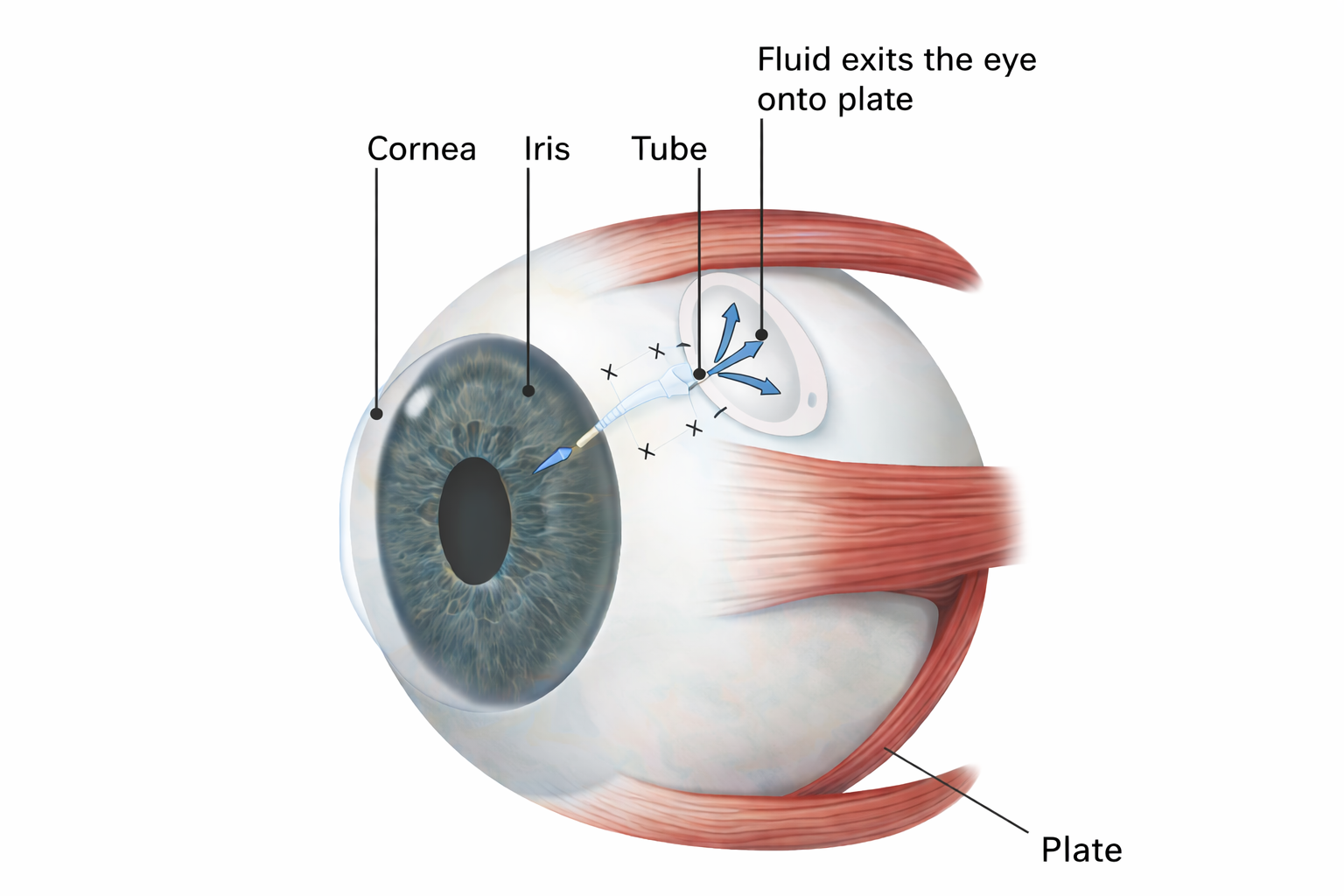
- Glaucoma Implants (Drainage Devices): Fine medical grade silicone tubes that are inserted into the front chamber of the eye to facilitate fluid drainage.
- Cataract Surgery or Lens Extraction Specifically in angle closure or angle closure glaucoma, cataract surgery or lens extraction widens the drainage angle and relieves the obstruction to fluid outflow from the eye. Cataract surgery can be performed on its own, or in combination with MIGS, trabeculectomy or glaucoma drainage devices, allowing optimal lowering of eye pressures.
When to Consider Surgery?
Glaucoma surgery becomes necessary when other treatments are no longer enough to keep eye pressure under control. Surgery is considered when:
- Visual fields continue to worsen.
- Greater optic nerve damage occurs.
- Non-surgical options no longer control the condition.
- Daily tasks, particularly driving, or clarity of vision at night become more difficult because of poorer vision.
- There is a sudden or gradual rise in eye pressure, such as with angle closure glaucoma.
"With early detection and attentive monitoring using precision diagnostic technology, we are able to protect the optic nerve and therefore preserve vision. No individual should lose their vision because if glaucoma is diagnosed early, it is eminently treatable."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
What is Glaucoma Surgery Like?
Glaucoma surgery is a day procedure performed under local anaesthesia, meaning you stay awake but your eye is completely numb and comfortable. During surgery, we create a tiny new drainage pathway, augmenting the existing drainage system in your eye to help fluid flow out more easily. This gentle adjustment helps lower eye pressure and protects the optic nerve from further damage.
Modern glaucoma procedures are precise, minimally invasive, and designed to promote a smooth recovery with minimal discomfort. Most patients are able to return home the same day and resume normal activities shortly after, following the doctor’s guidance.
What are the Benefits?
The main benefits of glaucoma surgery include:
- Better control of eye pressure
- Reduced reliance on daily eye drops or medication
- Lower risk of further vision loss
The goal of every glaucoma procedure is simply to preserve the vision you have today and help you continue seeing clearly for years to come.
How is Post-Treatment Care and Recovery after Glaucoma Surgery?
After glaucoma surgery, recovery is generally smooth with proper care. Mild discomfort or temporary blurred vision may occur but these symptoms usually improve within a few days. You will be given detailed post-procedure instructions and prescribed eye drops to support healing and stabilise eye pressure. Flying is usually allowed about one week after treatment,once we confirm that your eye is healing well. Regular follow-up visits are essential to monitor eye pressure and ensure stable recovery. Adhering to these steps helps maintain long-term results and preserves vision.
Glaucoma Surgery Aftercare
Use this timeline as a quick guide to know what to do & what to avoid, as your eyes heal.
Rest your eyes, limit screen time, avoid reading.
You can shower/wash hair, but avoid direct water into your eyes.
Resume driving or work once your vision feels stable.
Light exercise. Avoid gym workouts, heavy lifting or bending low.
You may use eye make-up, take care not to get irritation or infection.
Wear eye shields at night to prevent accidental rubbing.
Avoid direct tap water contact with the eyes.
Can resume strenuous exercise, swimming & sauna.
About Dr Errol Chan
Dr Errol Chan is Medical Director & Senior Consultant Ophthalmologist at Ascend Eye Clinic in Singapore. He is an experienced eye specialist, with more than 18 years of clinical experience and more than 10,000 eye surgical procedures. Dr Chan’s specialty interests are in the management of cataract, glaucoma and retinal diseases, as well as in vision correction with laser vision correction and implantable collamer lens (ICL) implants.
In the area of glaucoma treatment, Dr Chan manages both complex and routine cases, prioritising accuracy, safety, and patient-centred care. His interests are in the use of new eyedrop medication, minimally-invasive glaucoma surgery, glaucoma laser procedures and filtration surgery.
Dr Chan graduated MBBS from the National University of Singapore with placement on the Dean’s List, and completed Ophthalmology training at the National University Hospital in Singapore. Dr Chan further pursued international fellowship training at McGill University in Canada, and Moorfields Eye Hospital London in the UK, and stints at Great Ormond Street Hospital and Optegra Eye Hospital London in the UK.
Dr Chan is fellowship-accredited in Ophthalmology by the Royal Colleges of Edinburgh, Glasgow, London, Canada, and the Academy of Medicine Singapore.
He adopts a meticulous approach in consultation, surgical and follow-up care. Many patients, including those from Indonesia, seek consultation for second opinions or for specialized procedures using evidence-based and forefront medical technology.
To support Indonesian patients, his team provides Bahasa assistance and step-by-step guidance to ensure a smooth, comfortable experience from consultation to recovery.

Frequently Asked Questions (FAQs)
1. How is glaucoma treatment in Singapore different from Indonesia?
Treatment is individualised, based on the latest medical evidence and technology, and closely-monitored for long-term results. In Singapore, we have access to implants and medications that may not be available at your local eye specialist. Importantly, your overall glaucoma treatment will be supported by personlised care and technological advancements, in accordance with local and international clinical standards.
2. How do I know which treatment is right for me?
After a detailed eye assessment and personalised consultation, we will recommend the best option, whether it is medication, laser, surgery, or a combination of any of these, based on your eye condition.
3. How effective is laser treatment for glaucoma?
Laser procedures are highly effective for specific types of glaucoma. Laser treatments can significantly lower eye pressure, reducing the need for multiple eyedrop medications, and potentially delay the need for surgery.
4. How much does glaucoma treatment cost in Singapore?
The total cost depends on the type and stage of glaucoma, whether medical or surgical treatment or both are required, and the specific treatment modality. A consultation and detailed eye examination are needed before providing an accurate estimate. Please contact and tell us your case, to get an estimated cost.
5. How can Indonesian patients get treatment in Singapore?
Our Bahasa-speaking team in Indonesia helps with appointments, travel, and coordination, making it easy to access trusted care in Singapore.
6. Do I need to repeat eye tests in Singapore if I already had them done in Indonesia?
In most cases, yes. Even if you have previous results, Dr Chan usually repeats key eye tests to confirm eye pressure, optic nerve condition, and visual field status using clinic based equipment. This ensures treatment decisions for glaucoma are accurate and safe.
7. How long do I need to stay in Singapore for glaucoma treatment?
For consultations, laser procedures, or Minimally-invasive Glaucoma Surgery (MIGS), most patients only need to stay in Singapore for a few days. If more complex glaucoma surgery is required, a slightly longer stay may be advised to allow proper review before travel.
8. When is it safe to fly back to Indonesia after glaucoma treatment?
All patients are generally fit to fly home within 1–2 days after laser treatment, 3–4 days after Minimally-invasive Glaucoma Surgery (MIGS), and after 5-10 days after standard glaucoma filtration surgery. For more advanced glaucoma procedures, we will recommend the safest travel timing based on eye pressure stability and healing progress, to minimize any travel-related risks.
9. Will I need to stay overnight in the hospital after glaucoma surgery?
Most modern glaucoma surgery procedures are done as a day procedure, meaning you can return to your accommodation on the same day. Overnight stay is usually only needed in selected cases, depending on the type of surgery and individual recovery.
10. Will I still need eye drops after glaucoma surgery?
Some patients may still need eye drops after surgery, but often in lower doses of fewer number of eyedrop medications.
The goal of glaucoma surgery is to better control eye pressure and reduce dependence on long term medication, while protecting remaining vision.
To learn more or schedule your consultation, contact our Indonesia office via WhatsApp. We’re here to help you.




