Glaucoma is a common eye condition that affects the optic nerve and most often occurs in older adults. In its early stages, there are virtually no symptoms. It develops slowly and silently, gradually affecting side (peripheral) vision before central vision becomes impaired. The good news is, with timely diagnosis and treatment, many patients can preserve their sight and maintain a good quality of life.
What is Diabetic Retinopathy?
Diabetic retinopathy is a diabetes-related eye condition that affects the retina, the light sensitive layer at the back of the eye, that plays a vital role in vision. It develops when prolonged high blood sugar levels damage the small blood vessels that supply oxygen and nutrients to the retina.
In the early stages, vision may remain unaffected. However, without proper monitoring and management, the condition can worsen over time and lead to vision impairment and in severe cases permanent vision loss.
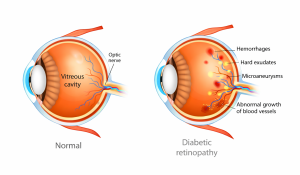
Stages of Diabetic Retinopathy
Diabetic retinopathy develops over time and is classified into two main stages. Each stage reflects the severity of blood vessel damage within the retina.
- Non-Proliferative Diabetic Retinopathy (NPDR)
This is the earlier stage of the condition where small blood vessels in the retina weaken or leak small amounts of fluid, but many patients do not experience noticeable vision changes as symptoms are often absent at this stage. Regular eye examinations play an important role in early detection and allows timely intervention to prevent further progression. - Proliferative Diabetic Retinopathy (PDR)
This is a more advanced stage of the disease. When blood supply to the retina is reduced, the eye responds by growing new abnormal blood vessels. These vessels are fragile and bleed more easily, increasing the risk of more severe vision problems such as vitreous haemorrhage, membranes and traction on the retina, retinal detachment, or even high eye pressures.
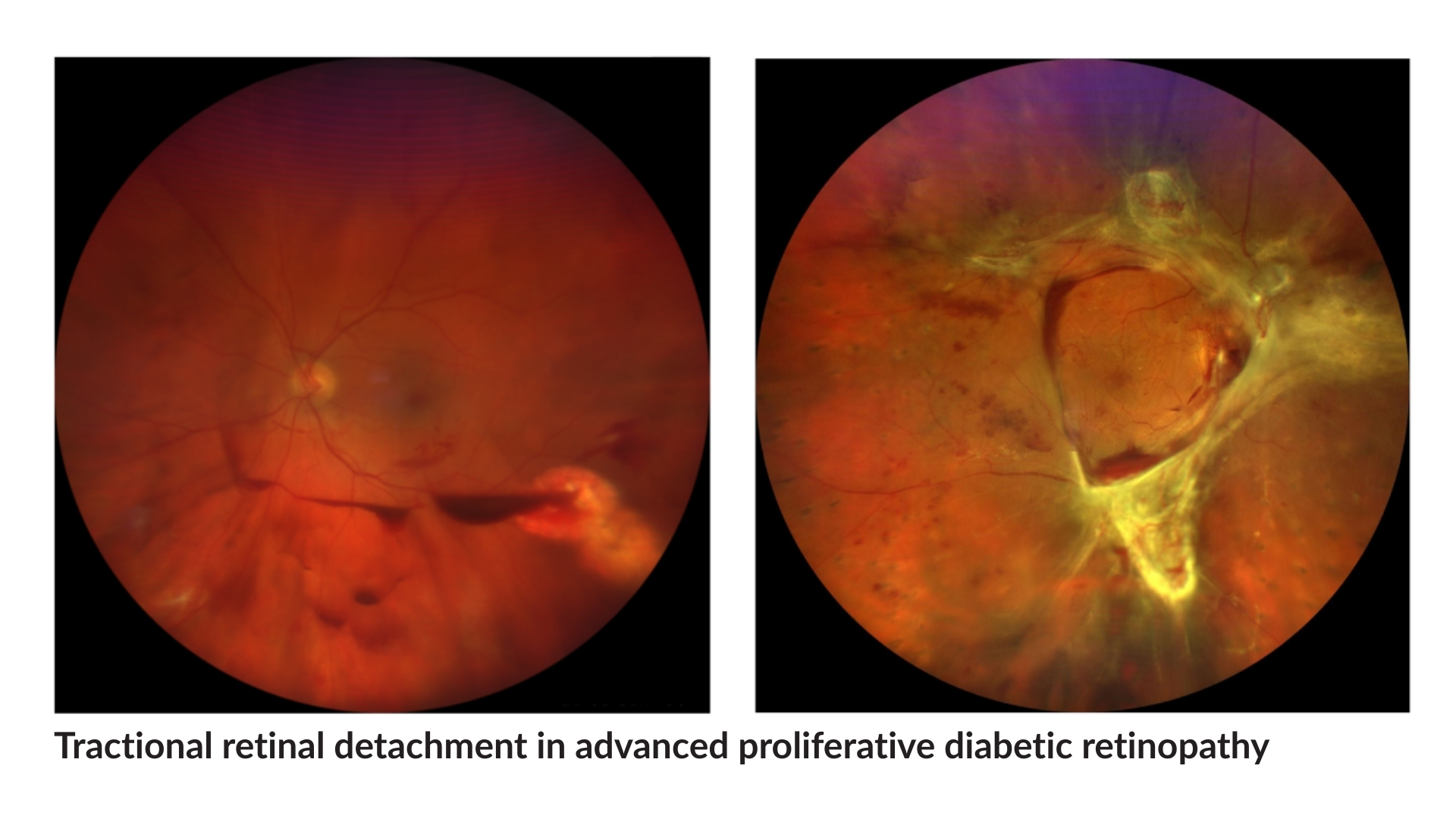
- Diabetic Macular Oedema (DMO)
When leakage occurs from the retinal blood vessels located in the central part of the retina, i.e. the macula, fluid accumulates amongst the important light-sensing cells responsible for fine and precise vision. This causes vision to become blurry or distorted.


Normal Vision
Loss of Peripheral Vision
"Diabetic retinopathy is a blinding condition, but with today’s retinal imaging technologies, early detection, timely intervention and ongoing meticulous monitoring, we can help patients achieve significant improvement of overall disease and optimise their vision."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
What Causes Diabetic Retinopathy?
The primary cause of diabetic retinopathy is long-term exposure to high blood sugar levels. Over time, excess glucose damages the retinal blood vessels, affecting their ability to function properly. This causes leakage and bleeding into the retina.
The risk increases with longer duration of diabetes, poor blood sugar control, high blood pressure, and elevated cholesterol levels. Careful management of these factors helps slow disease progression.
Symptoms of Diabetic Retinopathy
In many cases, diabetic retinopathy does not cause symptoms in its early stages. Vision changes often appear only after the condition has progressed.
Symptoms include:
- Blurred or distorted vision
- Dark spots, shadows, or “floaters” in the field of vision
- Difficulty seeing clearly at night or in low light
- Changes in colour vision
- Sudden changes in vision in more advanced stages
Because symptoms can be subtle or absent early on, regular eye screening remains important even when eyesight feels normal.

Floaters & Flashes of Light
Sudden appearance of spots, lines, or flashes may indicate changes in the retina and should not be ignored.

Distorted or Wavy Vision
Straight lines appearing bent or distorted can be a sign of macular or retinal conditions affecting central vision.

Blurry Vision
Gradual or sudden blurring of vision may occur when the retina is unable to transmit clear visual signals.
Diagnostic Assessment of Diabetic Retinopathy
In order to guide the most appropriate treatment, precision diagnostic assessment is essential. For diabetic retinopathy, the following diagnostic tools assist in determining optimal disease management:
- Ultra Wide-field Fundus Photography
- Spectral Domain OCT
- Fluorescein Angiography
- OCT Angiography
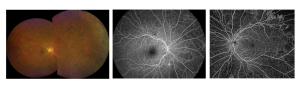
Treatment Strategies for Diabetic Retinopathy
Treatment depends on the severity of the diabetes in the eye, and whether complications of the primary condition have developed. The aim of treatment is to control diabetic retinopathy disease activity, manage and to prevent complications, and to improve and preserve vision.
At Ascend Eye Clinic in Singapore, we offer the following treatment strategies:
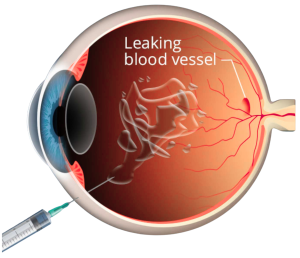
- Intravitreal Injections of Anti-VEGF or Sustained-Release Steroid Implants
Medications are delivered through eye injections to reduce retinal swelling and control abnormal blood vessel growth. These treatments are commonly used in moderate to advanced cases.
Several medication options are available, including longer-acting anti-VEGF injections that will allow for fewer treatment visits, and yet still maintain the same level of control of diabetes activity in the eye.
In cases where response to anti-VEGF treatment is limited, steroid implants can be considered as an alternative treatment option, with suitability also depending on the patient’s individual eye condition.
- Laser Treatment
There are several forms of laser treatment.
Panretinal photocoagulation is used to reduce abnormal blood vessel growth in the entire retina. This approach helps stabilise the condition and lowers the risk of further vision deterioration, and constitutes an important aspect of treatment lending stability to the condition if performed appropriately.
Macular grid and focal laser treatment targets fluid leakage and bleeding at the macula, which is the central part of the retina and responsible for fine and precise vision. The effectiveness can be slightly delayed for a few months, and is a useful adjunct to treatment besides intravitreal therapy.
- Surgical Treatment
In advanced cases, surgery is necessary when bleeding or scar tissue affect the retina or threaten vision. Surgical management of diabetic retinopathy requires careful judgement, precise technique, and experience in handling complex retinal conditions. Advanced cases often involve bleeding, scar tissue, or traction on the retina, which may coexist with other eye problems such as cataract or glaucoma. Management in these situations benefits from a retinal specialist with experience in both medical and surgical treatment planning, so that timing, approach, and follow-up care are appropriately coordinated. - Individualised Long-Term Care
Diabetic retinopathy often requires ongoing follow-up. Treatment plans are regularly reviewed and adjusted to maintain retinal stability and protect vision over time.
What Can I Expect after Diabetic Retinopathy Treatment?
Treatment aims to stabilise the diabetic retinopathy activity, achieve a more stable retina, and improve vision.
Early detection and expedient treatment will help achieve the most optimal outcomes and improvement of vision. Even with advanced disease, improvements are achievable with accurate diagnostic assessment and
As diabetic retinopathy is a long-term condition, regular post-treatment follow-up is required. Monitoring will involve consultation visits, where diagnostic testing such as macular OCT, fluorescein or OCT angiography, and Wide Field Fundus imaging will be performed to precisely assess your diabetic retinopathy status. Regular monitoring allows any further changes such as leakage or bleeding to be addressed appropriately, in order to protect vision over time.
"With advanced diabetic eye disease, patients can still achieve significant improvements in their eye condition and vision. At Ascend Eye Clinic, we adopt a meticulous diagnostic assessment with high-resolution retinal imaging, leverage on advancements in medications and surgical technology, and above all, provide personalised & attentive care, in order to help patients affected with diabetic retinopathy achieve the most optimal and sustainable outcomes after treatment."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Glaucoma Surgery Aftercare
Use this timeline as a quick guide to know what to do & what to avoid, as your eyes heal.
Rest your eyes, limit screen time, avoid reading.
You can shower/wash hair, but avoid direct water into your eyes.
Resume driving or work once your vision feels stable.
Light exercise. Avoid gym workouts, heavy lifting or bending low.
You may use eye make-up, take care not to get irritation or infection.
Wear eye shields at night to prevent accidental rubbing.
Avoid direct tap water contact with the eyes.
Can resume strenuous exercise, swimming & sauna.
About Dr Errol Chan
Dr Errol Chan is the Medical Director and Senior Consultant Ophthalmologist at Ascend Eye Clinic Singapore, with a subspecialty focus on medical and surgical retinal diseases, including diabetic eye disease and retinopathy.
With more than 18 years of clinical and surgical experience and over 10,000 eye procedures performed, Dr Chan provides comprehensive and individualised care for patients with routine and complex retinal diseases, from early diagnosis to long-term management.
Dr Chan obtained his medical degree (MBBS) with Distinction from the National University of Singapore and completed his ophthalmology specialist training at the National University Hospital, Singapore. He holds Ophthalmology specialist accreditations from the Royal Colleges in Edinburgh, Glasgow, London and Canada, as well as the Academy of Medicine, Singapore.
Dr Chan is an international triple fellowship-trained specialist in retinal diseases and retinal surgery. He was awarded a scholarship by the Retina Foundation of Canada to pursue a Vitreoretinal Surgery Fellowship at McGill University, Canada, and has also completed Advanced Vitreoretinal Surgery and Medical Retina & Uveitis Fellowships at the world-renowned Moorfields Eye Hospital London, UK.
In the management of diabetic eye disease, Dr Chan holds expertise in advanced imaging, intravitreal injections, photodynamic therapy, and surgery for complex and treatment-resistant disease. His management approach emphasises early detection, evidence-based treatment, clinical expertise and forefront technology to improve vision and support long-term retinal health.
As a retinal specialist, Dr Chan also manages various medical and surgical retinal diseases, such as diabetic eye disease, retinal detachment, macular hole, epiretinal membrane, retinal vascular and choroidal diseases, uveitis and inherited retinal diseases. He is frequently consulted for second opinions on complex retinal cases, including those involving Indonesian patients.
Dr Chan has authored more than 40 peer-reviewed journal publications and textbook chapters, presented at international Ophthalmology conferences, and participated as an investigator in international clinical trials advancing treatments for retinal disease. His work has been recognised with multiple international awards, including accolades from the Asia-Pacific Vitreoretinal Society.

Frequently Asked Questions (FAQs)
1. Do I need a referral to get checked?
No, you do not need a referral to make an appointment with us! You can contact us to book an eye assessment directly. We look forward to helping you achieve best control of your diabetic eye condition.
2. How often should diabetic patients have eye checks?
Diabetic patients who do not have diabetic eye disease require an eye examination once a year, at minimum. For patients with poorly controlled diabetes, examinations need to be more frequent than once a year. Additionally, for patients who already have diabetic eye disease our doctor may recommend more frequent visits depending on findings.
3. When should diabetic patients have an eye examination?
The American Academy of Ophthalmology and American Diabetic Association recommend that all Type 2 diabetics should have a dilated eye examination to detect diabetic changes in the eye at the point of diagnosis. Type 1 diabetics should have such an eye examination at latest 5 years after they are diagnosed.
Therefore, for diabetic individuals who have never had an eye examination, they should see an ophthalmologist to have an eye examination as soon as possible, and not wait until they experience any visual symptoms.
When visual symptoms in diabetic eye disease have developed, it is usually at an advanced stage of the disease, where more complex treatment is required, with a higher risk of losing vision and lower success rate of treatment.
4. I have advanced diabetic eye disease and I have been told that there is no hope for my condition. What should I do?
While advanced diabetic eye disease can be severe, it does not mean that no treatment is possible. An eye with proliferative diabetic retinopathy is eminently treatable, and it is important to recognise that appropriate and timely management decisions on medical and surgical treatment need to be made by an experienced retinal specialist, in order to achieve the best possible outcomes.
Effective treatment will stop progression of the disease to even more severe stages and prevent complications, such as development of high pressures or extensive tractional retinal detachment. Treatment will also preserve and may even improve vision slightly.
An assessment by a retinal specialist is important to determine what options are appropriate for your diabetic eye condition.
5. How many visits might be needed for treatment?
It depends on the severity of the disease in your eye. If there is no diabetic retinopathy or macular oedema present, then only monitoring, with regular eye examinations, is required. However, if there is diabetic retinopathy or diabetic macular oedema, then this would require treatment.
6. Can diabetic retinopathy be treated even if vision is still good?
Yes. Early treatment slows progression and protects vision, even when symptoms are mild or absent.
In severe or proliferative diabetic retinopathy, vision can still be good if there is little bleeding or leakage at the macula. Treatment, in the form of laser or intravitreal anti-VEGF injections, is still required to prevent progression of the disease. When the disease worsens, complications will develop. Also, in early stages of macular oedema, earlier treatment achieves better success, and reduces the need for multiple injections or laser treatments in the future.
7. I have a cataract and I have diabetic retinopathy. Can my condition be managed successfully?
Yes. Cataract and diabetic retinopathy can be managed successfully, and both conditions should be addressed carefully. The goal of treatment is to stabilise the diabetic eye disease while also improving vision through cataract removal.
Because these conditions can affect each other, it is important to be treated by an eye specialist who is experienced in both cataract surgery and medical and surgical retinal diseases.
In most cases, the diabetic retinal condition should first be stabilised before cataract surgery is performed. The timing of surgery depends on the clinical assessment of the retinal specialist, who will determine when the eye is sufficiently stable for a safe operation. In some cases, treatment for diabetic retinopathy may also be performed around the time of cataract surgery to reduce the risk of the condition worsening after the procedure. If cataract surgery is performed when the diabetic retinal condition is not sufficiently stable, it may lead to complications that require more intensive treatment.
8. Will treatment restore vision that is already lost?
Treatment aims to stabilise the diabetic activity in the eye, reduces leakage, and effectively preserves or improves vision.
A detailed assessment of your eye condition in a formal consultation with an experienced eye specialist will help advise the likelihood of vision improvement.
9. How long do I need to stay in Singapore for diabetic retinopathy treatment?
For assessment or injections, many patients only need a short 1 or 2 day stay. More advanced treatments may require additional follow up visits.
10. Can I fly back to Indonesia after eye injections or laser treatment?
Yes, there are no major issues with air travel after treatment. For eye injection or laser treatment, patients can fly home within the day. For retinal surgery, a short stay in Singapore of up to 4 to 7 days is required, with the duration of stay dependent upon your specific diabetic condition, the extent of surgery, and your progress during immediate post-operative follow-up.
11. Will I need repeated injections or treatments?
In the initial stages of treatment, especially for patients where eye disease is not optimally controlled, more regular treatment, in the form of intravitreal injections or laser, is required. With improvement in disease activity, less frequent treatment to no treatment may be required eventually. Therefore, it does not mean that patients with diabetic eye disease require life-long treatment.
12. What tests are usually repeated during follow up visits?
Follow up may include OCT, retinal imaging, or angiography to monitor retinal swelling and blood vessel changes.
13. What should I prepare before my visit?
Bring your recent diabetes-related results if available (e.g., HbA1c), a list of medications, and any past eye reports or scans.
To learn more or schedule your consultation, contact our Indonesia office via WhatsApp. We’re here to help you.




