A sudden increase in floaters, flashes of light, or a dark “curtain” in your vision can be more than just a temporary disturbance. These can be early warning signs of retinal detachment, a condition that needs urgent eye assessment to protect your sight. With early diagnosis and appropriate treatment, many cases of retinal detachment can be successfully managed, allowing patients to preserve useful vision and prevent permanent visual loss.
What is a Retinal Detachment?
Retinal detachment occurs when the retina, the thin, light-sensing layer at the back of the eye, separates from the eye wall and can no longer function properly. As this separation progresses, vision often becomes blurred, shadowed, or may deteriorate rapidly.
The condition is usually painless, which can delay medical attention , especially if symptoms affect only one eye or the non-dominant eye. Despite the lack of pain, a retinal detachment is considered an eye emergency. Early diagnosis and prompt treatment offer the best chance of preserving vision.
Seek urgent eye care if you notice:
- A sudden increase in floaters (spots, lines, dust, or threads in the vision)
- Flashing lights
- A shadow or curtain in your peripheral vision that spreads toward the centre
- Central vision loss as the central retina becomes involved
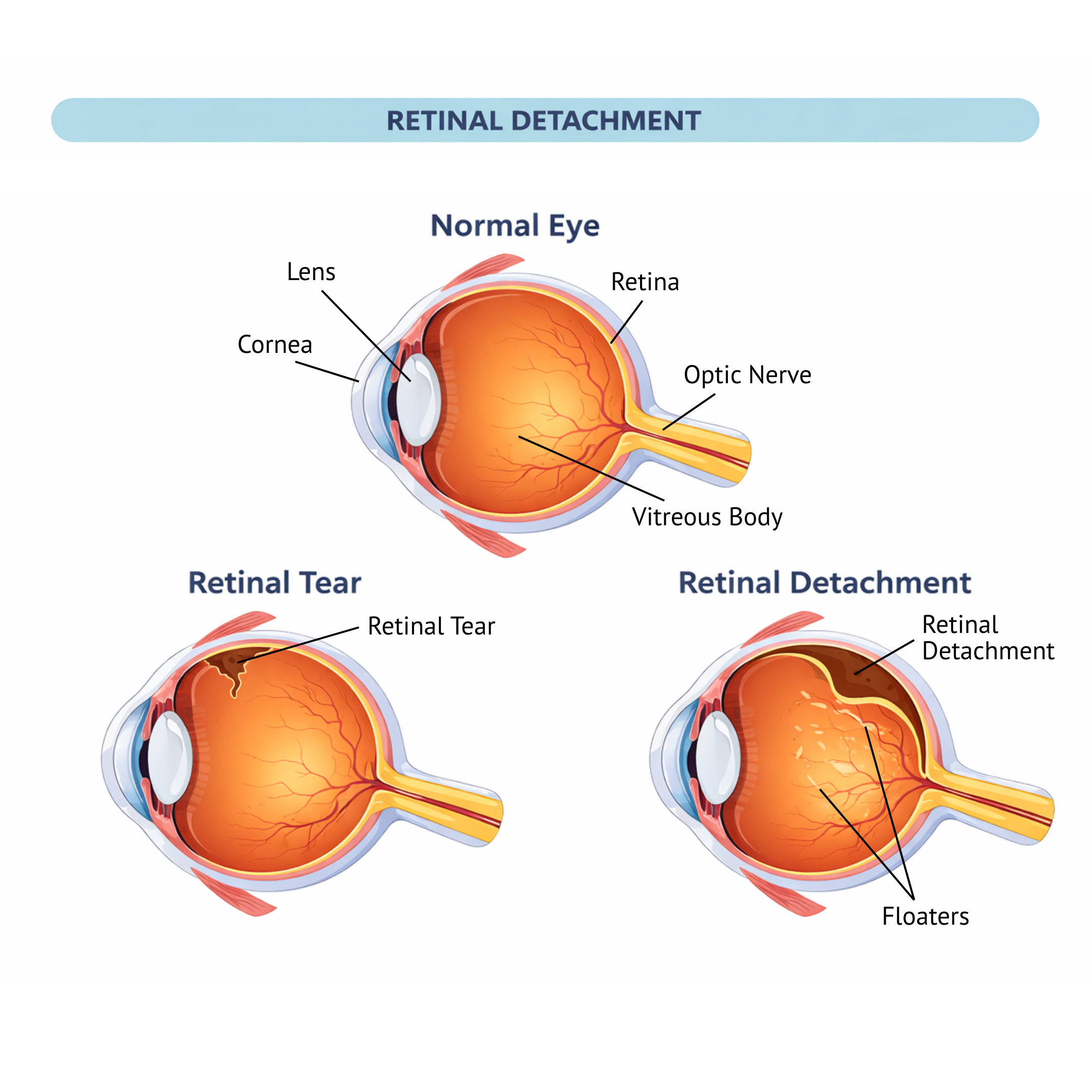


Normal Vision
Loss of Peripheral Vision
"It is important to note that early or slowly progressing retinal detachments give little to no symptoms. Thus having a regular or at least a baseline eye assessment to determine the retinal status is an important step to safeguarding your vision."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Causes & Types of Retinal Detachment
Retinal detachments are grouped into three main types, based on what causes the retina to lift away from the back of the eye.
1. Rhegmatogenous Retinal Detachment
Cause: A tear or hole in the retina, often linked to age-related vitreous changes (posterior vitreous detachment), high myopia (severe short-sightedness), or an eye injury.
What happens: Fluid slips through the retinal tear and collects under the retina, causing it to separate from the eye wall (like wallpaper peeling off the wall). 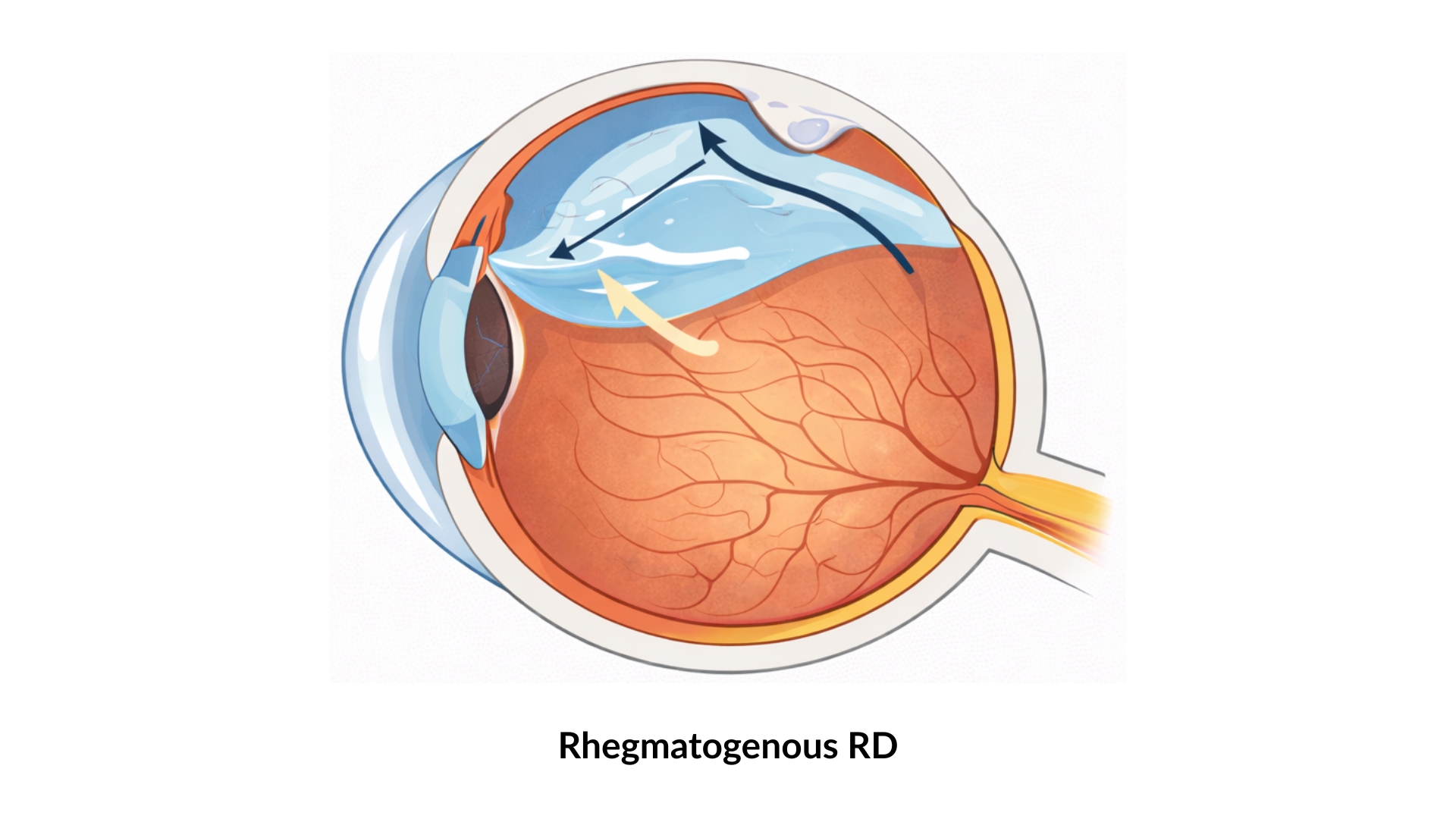
2. Tractional Retinal Detachment
Cause: Scar tissue on the retinal surface, most commonly from advanced diabetic eye disease. The scar tissue tightens and pulls the retina away from the wall of the eye.
What happens: If the pull is sufficiently strong, the retina separates away from its attachment to the wall of the eye, causing a retinal detachment.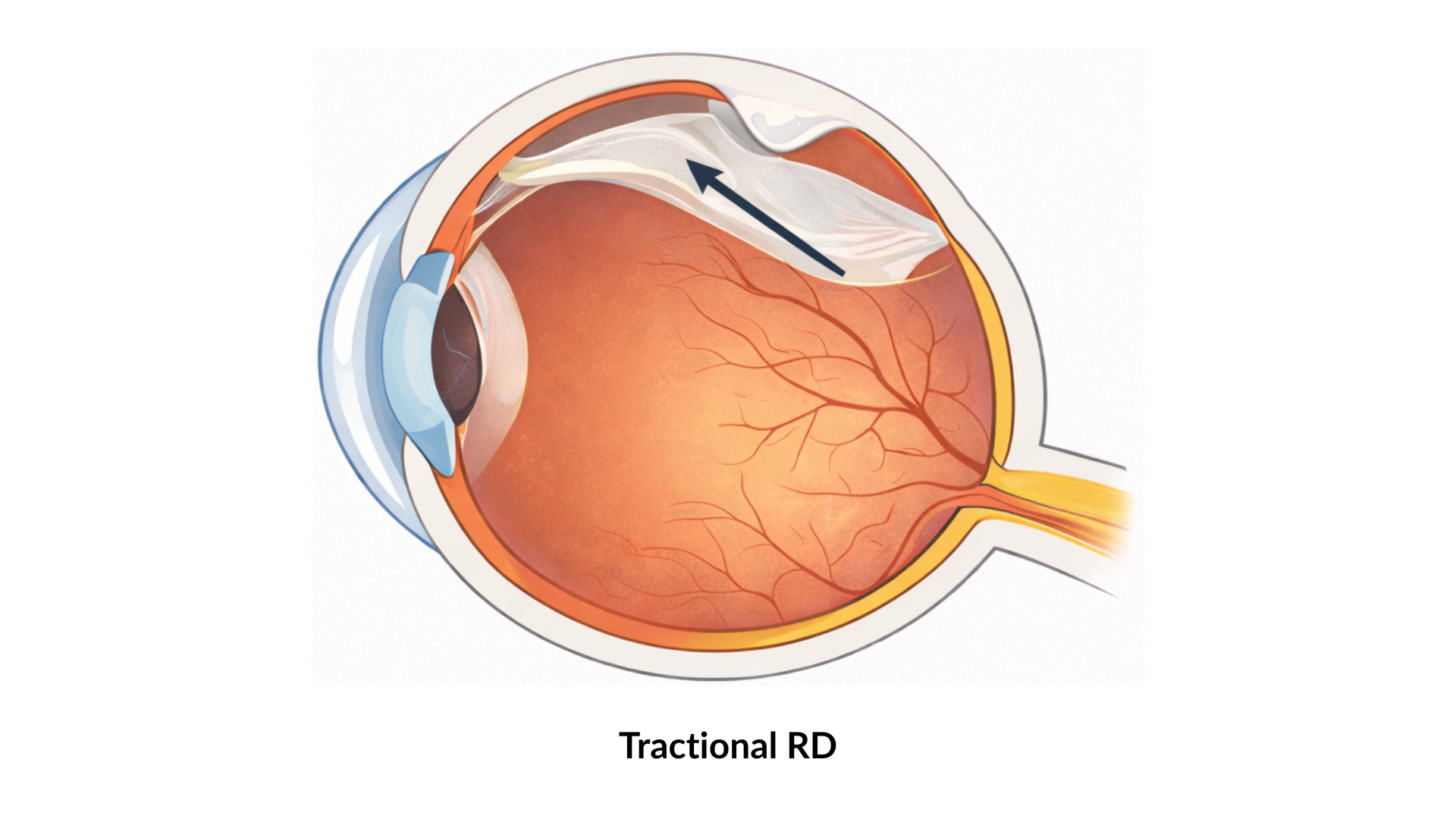
3. Exudative Retinal Detachment
Cause: Fluid leakage beneath the retina due to conditions such as inflammatory eye disease (i.e. uveitis) or leakage from the retinal or choroidal blood vessels.
What happens: Fluid builds up beneath the retina without a retinal hole or tear, causing the retina to separate from the eye wall.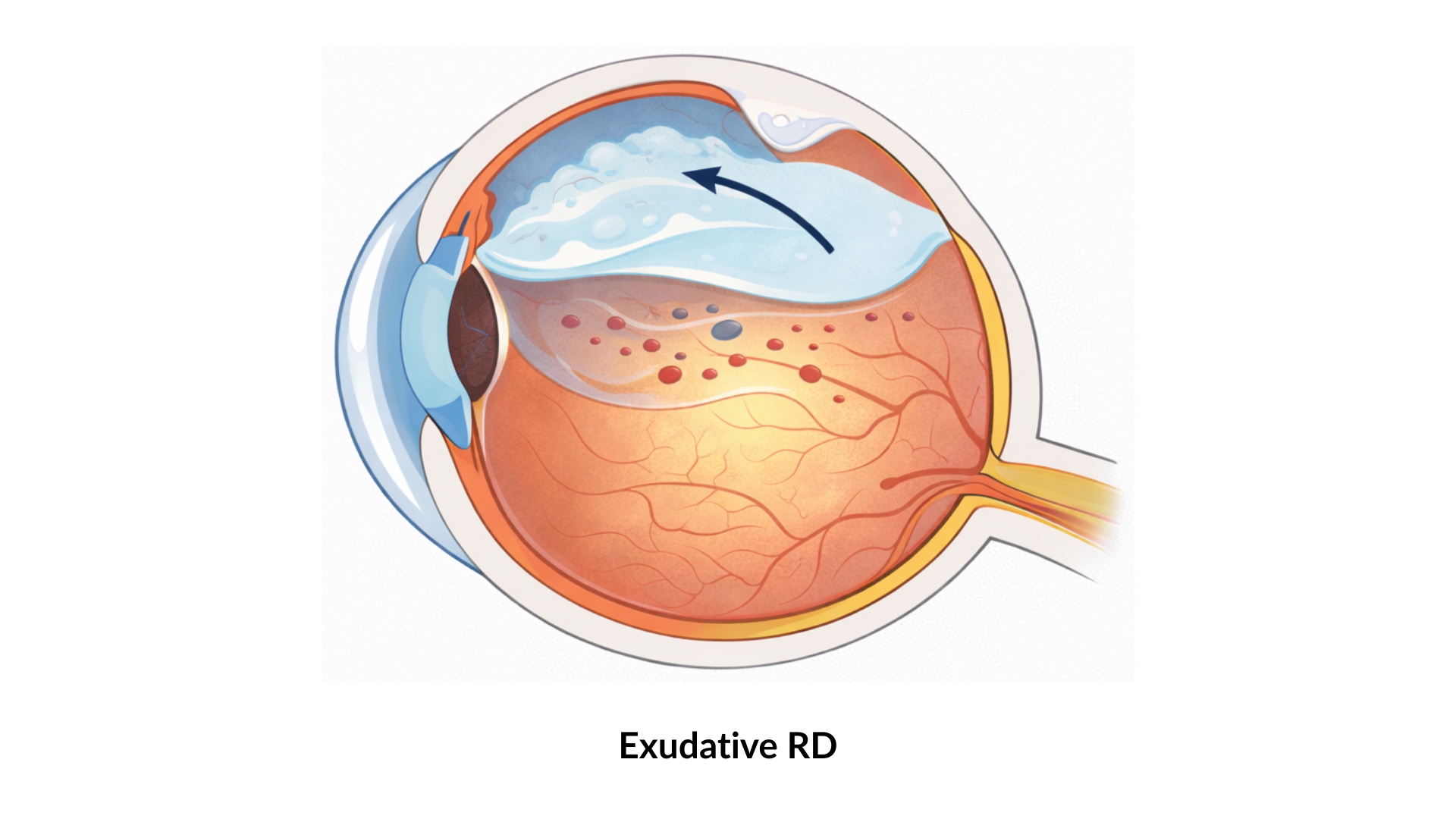
Am I at Risk for a Retinal Detachment?
Retinal detachments can affect anyone, but certain factors increase the risk. The likelihood of a detachment increases with age, as natural changes in the vitreous gel place stresses on the retina. The following factors increase the risk for a rhegmatogenous retinal detachment:
- Posterior vitreous detachment: this is the most common cause. As the gel contracts with increasing age, it may pull on the retina strongly enough to cause a retinal tear. The retinal tear being open will lead to fluid passage into itself, causing a retinal detachment, where the retina lifts off from the wall of the eyeball.
- Lattice degeneration, which are thin areas in the retina predisposing to retinal tears. As these do not give visual symptoms, they can only be detected on a dilated eye examination by an eye specialist.
- High myopia, which leads to long eyeball length and a thinner retina, more susceptible to tears.
- Previous eye injuries.
- Prior eye surgery, such as cataract surgery.
- Retinal detachment in the the other eye.
- Family history of retinal detachment
For tractional retinal detachments, the following factors increase the risk of its occurrence:
- Diabetes or other retinal diseases with scarring in the retina, as scar tissue tugs on to retina, causing it to separate.
- Prior eye injury with scarring.
- Retinal conditions from childhood
If you have one or more risk factors, going for regular eye examinations is important. Early detection of retinal changes allows timely treatment and helps reduce the risk of serious vision loss.
Retinal Detachment Treatment
The main goal of retinal detachment treatment is to reattach the retina and seal any tears or holes that have caused it. Several treatment options are available, and the most appropriate approach depends on the type, extent and severity of the detachment, overall prognosis, and individual factors such as age, requirement for air travel, and ability of the patient to adopt specific head positioning postures.
A retina specialist will assess these factors carefully and recommend the treatment that offers the best chance of preserving vision. Modern surgical techniques allow many retinal detachments to be repaired successfully, particularly when treatment is carried out promptly.
- Vitrectomy Surgery
Vitrectomy is a microsurgical procedure where the vitreous gel inside the eye is removed. Fluid trapped beneath the retina is drained, and retinal tears are sealed using laser treatment or freezing therapy (cryotherapy). If there is significant retinal scarring (i.e. proliferative vitreoretinopathy, PVR), then this can be removed. A gas bubble or silicone oil is then placed in the eye to support the retina in position while it heals. - Scleral Buckling Surgery
A soft silicone band is placed around the outside of the eye to gently push the eye wall inward, helping the retina reattach. Retinal tears are sealed with laser or cryotherapy treatment, and in some cases, fluid under the retina is drained. A small gas bubble may also be placed in the eye to provide additional support to the retina for its reattachment. - Pneumatic Retinopexy
A gas bubble is injected into the eye during a clinic-based procedure. The patient maintains a specific head position so the bubble supports the retinal tear. The tear is then sealed with laser or cryotherapy treatment and this allows a permanent seal of the tear. This approach may be suitable for selected cases where the retinal breaks are in the upper parts of the retina, and is therefore considered as an alternative to vitrectomy surgery. - Laser Treatment
Laser therapy is used to create a controlled barricade around the affected area, preventing the retinal detachment from spreading. Laser treatment alone is usually considered for small, peripheral retinal detachments. - Combined Vitrectomy and Scleral Buckling Surgery
In complex retinal detachments or detachments with high-risk features for failure, both procedures may be necessary to enhance the success rates of retinal reattachment surgery.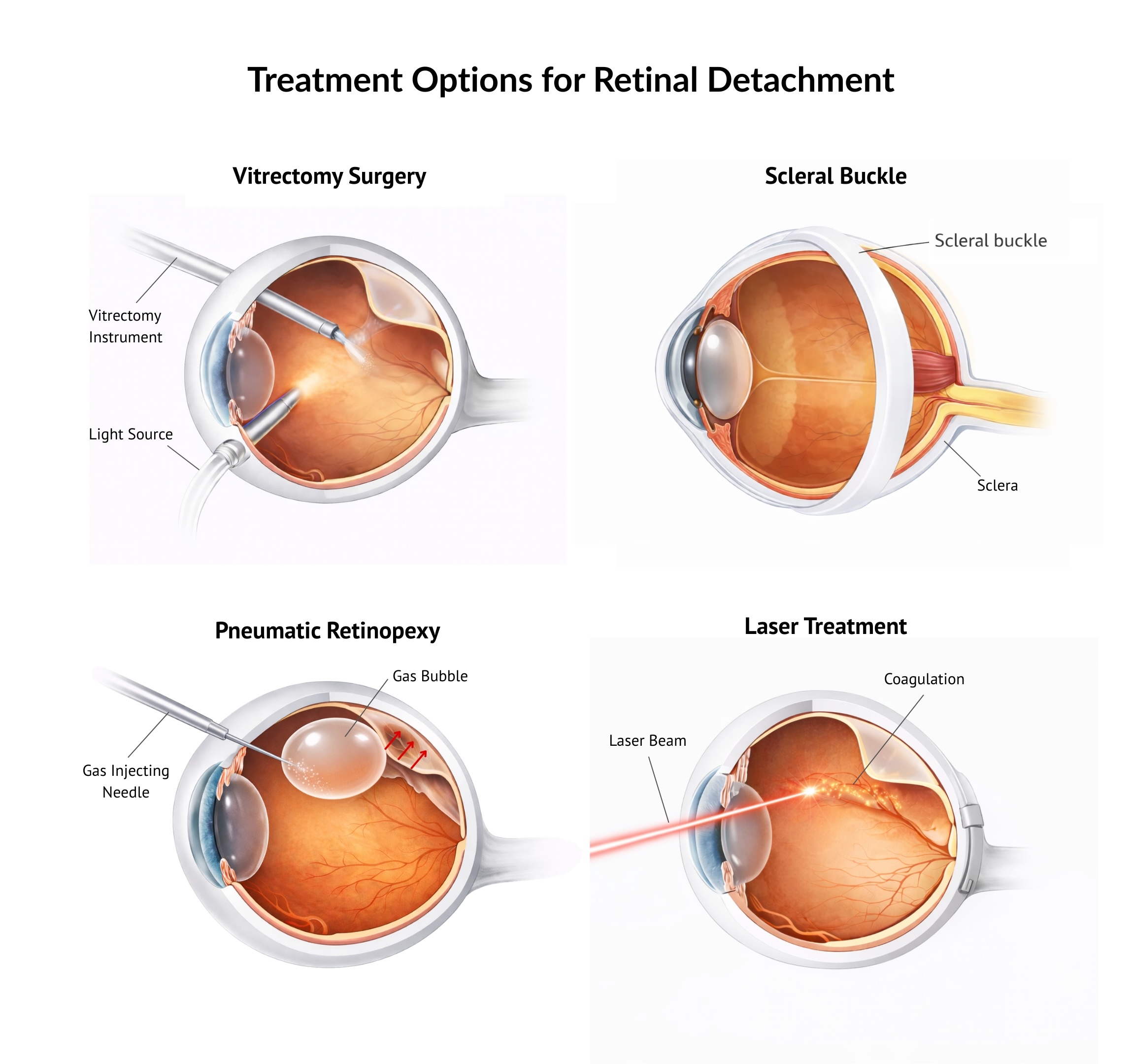
"For every patient experiencing a retinal detachment, there is the real prospect of losing sight permanently. As a specialist retinal surgeon, my priority is not only to provide the most optimal surgical management based on advanced surgical technology, but also to journey with the patient throughout treatment and recovery. A retinal detachment is certainly treatable. If managed promptly and appropriately, patients can expect to regain a large part of the vision that was initially lost."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Why Timely Treatment Leads to Successful Outcomes?
When retinal detachment is diagnosed and treated early, patients can experience several important benefits:
- Prevention of permanent vision loss
Prompt treatment helps stop the detachment from spreading and protects the central retina, which is essential for clear vision. - Better visual recovery
When treatment is done before the macula is affected, patients have a very high chance of retaining good visual clarity after surgical treatment. - High success rates with modern techniques
Advances in the technology used in retinal surgery mean most retinal detachments can be successfully repaired with a single procedure. - Reduced risk of complications
Early intervention lowers the chance of long-term complications, such as severe vision impairment or repeat detachments. - Preservation of daily function and independence
Maintaining vision supports everyday activities like reading, driving, and working, helping patients maintain quality of life.
Complex Retinal Detachments
Some retinal detachments are more difficult to treat due to excessive scarring of the retina, known as proliferative vitreoretinopathy (PVR). Scar tissue can form on or beneath the retina, preventing it from reattaching normally.
These complex cases are more likely in the presence of large or multiple retinal tears, giant retinal tears, bleeding inside the eye, eye injuries, choroidal detachment, or multiple previous eye surgeries. As a result, surgery becomes more technically demanding and requires careful planning.
Some patients with complex retinal detachments may have undergone prior operations and have been told that no further treatment is possible. In many situations, this reflects the complexity of the condition, rather than a lack of potential options. With detailed assessment and a tailored surgical approach by a retinal surgeon with strong clinical expertise, further treatment can usually still be considered to stabilise the retina and to preserve remaining vision.
"The success of every retinal detachment procedure depends critically on the surgeon making timely and appropriate surgical decisions, and in selecting the most appropriate technologies in treatment management. At Ascend Eye Clinic, we prioritize clinical experience, surgical expertise and technological leverage, to help patients with retinal detachments achieve the most optimal outcomes from treatment."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Aftercare & Recovery After Treatment
Successful retinal detachment treatment does not end in the operating room. Careful post-treatment management plays an important role in stabilising the retina, supporting healing, and protecting long-term vision.
An important part of recovery is head positioning, where patients are asked to keep their head in a specific position, such as face down or resting on the left or right side, for a period of time. This positioning helps the retina heal in the correct position. The duration varies depending on the surgical approach and individual healing, and may range from one day to a week or longer.
In some surgeries, a gas bubble is placed inside the eye to support retinal healing. When gas is used, air travel must be avoided until the bubble has completely dissolved, which may take several weeks. For Indonesian patients who need to travel home soon after surgery, silicone oil can be used instead of gas in selected cases. Silicone oil provides internal retinal support while allowing safe air travel.
Patients are given clear instructions and a structured follow-up plan to monitor healing and address any concerns. The timeline below outlines the general precautions and expectations during each stage of recovery.
Retinal Detachment Treatment Aftercare
Use this timeline as a quick guide to know what to do and avoid, and what to expect as your eyes heal.
Avoid rubbing or pressing on the eye. Maintain face positioning as directed.
Avoid direct contact of the eye with tap water.
Can return to light excercise.
Avoid swimming or strenuous physical activity.
Avoid dusty environments that may irritate the eye.
Usage of eyedrops to aid in healing.
Improve vision.
About Dr Errol Chan
Dr Errol Chan is the Medical Director and Senior Consultant Ophthalmologist at Ascend Eye Clinic Singapore, with a subspecialty focus on medical and surgical retinal diseases, including retinal detachment.
With more than 18 years of clinical and surgical experience and over 10,000 eye procedures performed, Dr Chan provides comprehensive and individualised care for patients with routine and complex eye diseases, from early diagnosis to longer-term management.
Dr Chan obtained his medical degree (MBBS) with Distinction from the National University of Singapore and completed his ophthalmology specialist training at the National University Hospital, Singapore. He holds Ophthalmology specialist accreditations from the Royal Colleges in Edinburgh, Glasgow, London and Canada, as well as the Academy of Medicine, Singapore.
Dr Chan is an international triple fellowship-trained specialist in retinal diseases and retinal surgery. He was awarded a scholarship by the Retina Foundation of Canada to pursue a Vitreoretinal Surgery Fellowship at McGill University, Canada, and has also completed Advanced Vitreoretinal Surgery and Medical Retina & Uveitis Fellowships at the world-renowned Moorfields Eye Hospital London, UK.
In the management of retinal detachments, Dr Chan holds expertise in surgery for routine and complex detachments, such as cases with previously failed procedures, or cases deemed inoperable by other retinal surgeons. He performs the full spectrum of surgical procedures to treat retinal detachment, such as vitrectomy, scleral buckle, laser and pneumatic retinopexy. His management approach emphasises meticulous assessment, clinical and surgical excellence, leveraging on forefront technology, in order to provide the most optimal outcomes for patients.
As a retinal specialist, Dr Chan manages various medical and surgical retinal diseases, such as diabetic eye disease, macular hole, epiretinal membrane, retinal vascular and choroidal diseases, uveitis and inherited retinal conditions. He is frequently consulted for second opinions on complex retinal cases, including those involving Indonesian patients.
Dr Chan has authored more than 40 peer-reviewed journal publications and textbook chapters, presented at international Ophthalmology conferences, and participated as an investigator in international clinical trials advancing treatments for retinal disease. His work has been recognised with multiple international awards, including accolades from the Asia-Pacific Vitreoretinal Society.
Frequently Asked Questions (FAQs)
1. Is retinal detachment an emergency?
Yes. Retinal detachment is considered an eye emergency. Early assessment and treatment are important to prevent permanent vision loss.
Early assessment and treatment are important to prevent permanent vision loss. If you experience any of such emergency symptoms, our team is experienced to be able to assist you for urgent treatment in Singapore, at short notice.
From the time you contact us and have your first consultation with us in Singapore can be as short as 6 hours, including flight travel time. We will be able to arrange surgery for you within 1-2 hours of your consultation with us.
Do contact our staff for further enquiries
2. How soon should I seek treatment after symptoms appear?
As soon as possible. Earlier treatment improves the chance of preserving useful vision, especially before the central retina is affected.
3. Will I need surgery for retinal detachment?
All cases of retinal detachments require laser or surgery. For selected cases of small detachments, surgery may be avoided if no visual symptoms are present. However, laser retinopexy is still required to safeguard extension of the retinal detachment
4. How long does retinal detachment surgery take?
Laser procedures are relatively quick, requiring between 10 to 15 minutes for each detachment. Surgical procedures take anywhere between 1 to 2 hours, depending on the complexity of the detachment, and the specific surgery performed. If combined vitrectomy and scleral buckling is performed, then surgical time will be longer.
5. How long is the recovery period after surgery?
The recovery varies between individuals and we would be able to advise you more specifically after a consultation visit.
In general, for patients undergoing vitrectomy or scleral buckling surgery, personal mobility is usually more limited initially due to the need to maintain head positioning for a specific minimum number of hours each day. After restrictions on head positioning are lifted, most patients are able to resume light activities immediately.
In terms of the initial visual recovery, this varies between individuals, depending on whether gas or oil was used, and in the case of gas, the duration in which the gas remains in the eye. The extent of longer-term visual recovery is dependent on the amount of damage sustained by the macula, from the time that the retina stayed detached, and on the overall complexity of the retinal detachment. Therefore, early and expedient treatment is important.
6. Will I need to maintain face down or side positioning after surgery?
Patients with gas or oil in the eye would require face down or side positioning after surgery, to support retinal attachment and healing, for a specific number of hours each day, shortly after surgery. The specific head positions and durations required will be advised following the surgical procedure.
7. Do I need to stay in Singapore for long after treatment?
The length of stay depends on the specific procedure(s) performed and your recovery progress. We will be able to advise on when it is safe for you to fly back, and when you should come in again for a review.
There is no restriction on air travel for patients with oil in the eye. Thus, as early as 3-4 days after vitrectomy surgery with oil placement, and post-operative review visits, patients will be able to fly back if they so require
8. Will I need further treatment or follow up after surgery?
Yes. Following an extensive and major surgery, it is important that to ensure the best possible outcomes, regular monitoring needs to be done. You would expect to fly back to Indonesia about 4-7 days after such surgery. Follow-up post-operative visits are usually scheduled at approximately 1 month and 3 months after surgery. If your travelling schedule is tight, modifications can always be made to fit your timings.
9. How to book a consultation?
To arrange a consultation with Dr Errol Chan, please contact us via WhatsApp. Our team will answer your questions and coordinate your appointment schedule in Singapore.
10. Will there be Indonesian assistance?
Yes. Bahasa Indonesia Patient Assist support is available to help with scheduling, coordinating your visit and treatment in Singapore, and answering practical questions before and after your appointment.
To learn more or schedule your consultation, contact our Indonesia office via WhatsApp. We’re here to help you.




