You notice it when you’re reading a message or looking at a familiar face appears slightly blurred, or straight lines start to look wavy, it is easy to attribute these changes to fatigue or normal aging. However, changes like this especially after age 50 can be a sign of age-related macular degeneration (AMD). The important thing is this: AMD can progress quietly, and the sooner it’s checked, the more we can do to protect your central vision.
What is Age-Related Macular Degeneration (AMD)?
Age-related macular degeneration is an eye condition that affects the macula, the central portion of the retina responsible for sharp, detailed vision. When the macula becomes damaged, activities such as reading, driving, or recognising faces become increasingly difficult.
AMD is one of the leading causes of vision impairment among people aged 50 and above. While peripheral (side) vision is usually preserved, the loss of central vision can significantly impact independence and quality of life.
Who is at Risk?
Age-related macular degeneration becomes more common as we grow older, particularly after the age of 50. However, certain factors may increase the likelihood of developing AMD.
You may be at higher risk if you:
- Have a family history of AMD
- Smoke or have smoked in the past
- Have high blood pressure or cardiovascular disease
- Are overweight
- Have prolonged exposure to sunlight without adequate eye protection
While these risk factors increase the chance of developing AMD, they do not mean you will definitely develop the condition. Regular eye examinations are especially important if you fall into any of these groups, as early detection allows closer monitoring and timely treatment when necessary.
Types of AMD
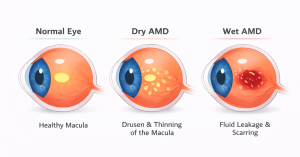
- Dry AMD is the more common form. It develops gradually as the macula thins and small deposits called drusen accumulate beneath the retina. Vision loss tends to be slow but progressive.
- Wet (Neovascular) AMD, although less common, but more aggressive and leads to vision loss more rapidly. It occurs when abnormal blood vessels grow beneath the macula and leak fluid or blood. This can lead to rapid and severe loss of central vision if not treated promptly.
Early detection is critical, especially for wet AMD, where timely treatment can make a meaningful difference in preserving your vision.
Recognising the Symptoms Early
Clear symptoms of AMD do not always appear suddenly. Many patients initially notice:
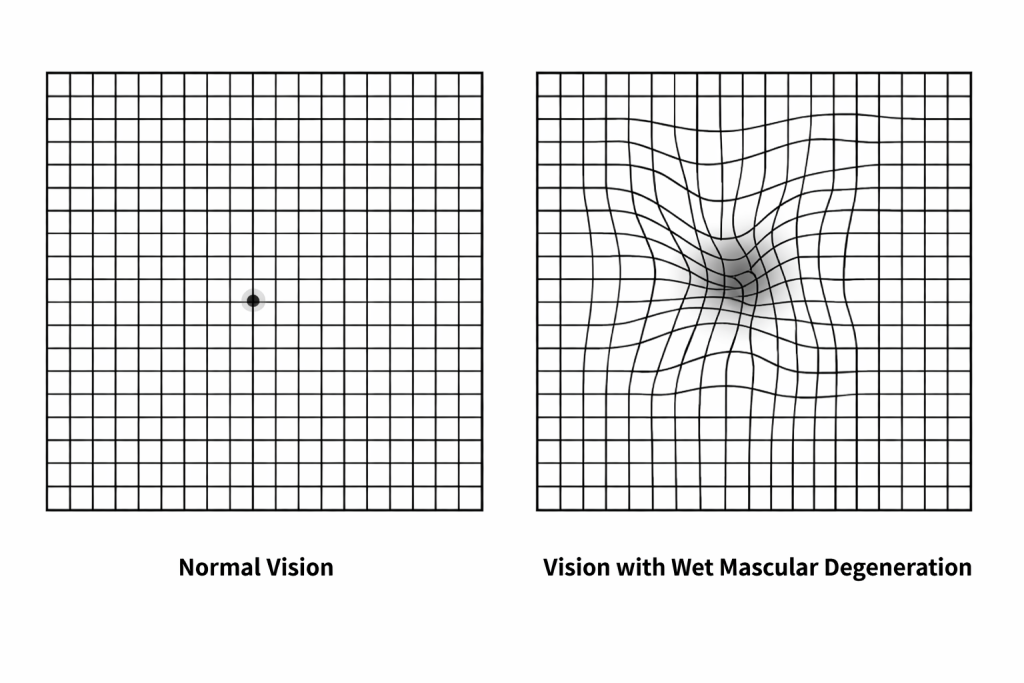
- Blurred or distorted central vision
- Straight lines appearing wavy or broken
- Difficulty reading or recognising faces
- A dark or empty spot in the centre of vision
 Because these changes may start in one eye, the brain often compensates, delaying diagnosis. Therefore unless the vision in each eye is checked separately, the individual may not notice anything untoward about their vision. Regular eye checks are essential, particularly if you are over 50 or have a family history of AMD.
Because these changes may start in one eye, the brain often compensates, delaying diagnosis. Therefore unless the vision in each eye is checked separately, the individual may not notice anything untoward about their vision. Regular eye checks are essential, particularly if you are over 50 or have a family history of AMD.
"Retinal conditions can be challenging to navigate. I believe in taking an empathetic approach, providing clear explanations and allowing patients the time they need to make informed decisions. Treatment plans are always discussed collaboratively, with the patient’s best interests as the top priority."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Imaging Assessment of AMD
At Ascend Eye Clinic in Singapore, we prioritise utilising multimodal diagnostic imaging to optimise planning and management of your AMD condition. These detailed scans allow us to evaluate both the structure and activity of the retina in detail, helping to guide personalised treatment decisions.
Our comprehensive diagnostic assessment includes:
- Spectral domain optical coherence tomography
- OCT angiography
- Fundus autofluoresence
- Fluorescein angiography
- Indocyanine green angiography
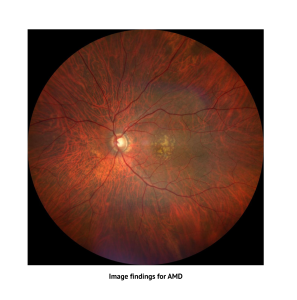
Several retinal conditions may appear to be AMD, but may not necessarily be AMD. By using various cross-sectional and angiographic imaging modalities, we can accurately differentiate these conditions, determine disease activity, and the true status of the retina. This thorough diagnostic approach ensures that treatment is both appropriate and optimally tailored to each patient’s condition.
Treatment Options for AMD
For patients with AMD, specific treatment depends on whether the condition is dry or wet.
Dry Age-Related Macular Degeneration
Dry AMD may not progress significantly, but if it does, it progresses gradually. The majority of patients with dry AMD continue to enjoy reasonably good vision. Overall, the treatment for dry AMD focuses on slowing disease progression, supporting retinal health and preserving vision.
Depending on the stage of dry AMD, different treatment options may be considered. For intermediate dry AMD, vitamin and supplement formulations such as AREDS2 help reduce the risk of disease progression to advanced dry AMD. This formulation contains vitamin C, vitamin E, zinc, lutein, and zeaxanthin. In individuals with advanced dry AMD (i.e. geographic atrophy), supplementation with this formulation also reduces the risk of progression and preserves vision.
In individuals with early to intermediate dry AMD and at high risk of progression, a non-invasive, low-intensity photobiomodulation laser therapy, a recently FDA-authorised treatment, is effective to help slow disease changes. This device delivers precise wavelengths of light to the affected retinal cells, enhancing their metabolic activity and promoting healing. This helps reduce the build-up of waste products of metabolism in the retina, and improves vision and contrast sensitivity.
For advanced dry AMD, newer intravitreal medications targeting the complement pathway, known as anti-complement factor inhibitors, may help slow progression and preserve vision. These are performed in the clinic under local anaesthesia.
Currently, we are now able to treat patients with dry AMD with various targeted treatment strategies, when previously, there were no effective treatments for this condition. For every patient with dry AMD, we individualise treatment accordingly, so patients may receive more than one form of treatment.
Wet Macular Degeneration
Wet age-related macular degeneration (AMD) progresses more quickly, but effective treatments are available to control the condition and protect central vision.
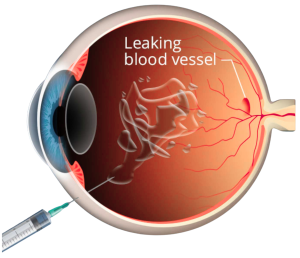
Intravitreal anti-VEGF injections are the main treatment for wet AMD. They are performed in-clinic under local anaesthesia and help reduce abnormal blood vessel growth and fluid leakage. Newer medications may allow for fewer injections over time while maintaining good control of the disease.
In selected cases, photodynamic therapy (PDT) may be recommended. This targeted treatment uses a light-activated medication and a specialised laser to treat abnormal blood vessels while preserving surrounding healthy tissue. This strategy is particularly important in cases of polypoidal choroidal vasculopathy, a variant of wet AMD occurring more commonly in Asians.
For more advanced wet AMD cases with significant bleeding in the macula, vitrectomy surgery & displacement of submacular haemorrhage may be considered to move blood away from the central retina, helping to reduce further damage and support visual recovery. This procedure is time-sensitive and early recognition of patients who would benefit from this is important, so that the opportunity to treat is not lost. Successful displacement of the blood effectively and rapidly restores vision in what would have been loss of central vision.
"At Ascend Eye Clinic, we place a priority on helping patients with age-related macular degeneration achieve their best possible vision, through a meticulous diagnostic assessment using forefront imaging platforms, access to a broad range of novel drug treatments, and expedient surgical treatment when required. This allows us to treat the condition effectively, promptly and safely, helping patients to achieve their best possible vision."
— Dr Errol Chan —
Medical Director & Senior Consultant Ophthalmologist
Ascend Eye Clinic, Singapore
Polypoidal Choroidal Vasculopathy
Polypoidal choroidal vasculopathy (PCV) is a retinal condition affecting the choroidal blood vessels beneath the retina. It is characterised by clusters of abnormal, aneurysm-like vessels that can cause fluid leakage or bleeding, leading to changes in vision.
PCV is often considered a subtype of wet AMD, as both conditions involve abnormal blood vessel growth and share similar symptoms. These include blurred or distorted central vision, dark spots, or sudden visual changes.
Because PCV can closely resemble AMD, accurate diagnosis is essential. Detailed retinal imaging such as OCT, fluorescein angiography, and indocyanine green angiography, helps identify disease activity and distinguish PCV from other retinal conditions.
For PCV, treatment commonly involves anti-VEGF injections to control leakage and disease activity. In selected cases, photodynamic therapy (PDT) may be used in combination to improve long-term outcomes and reduce the risk of vision loss.
How are Intravitreal Injections Performed?
The procedure is minimally invasive and performed in a clinic setting. Before the injection, the eye is thoroughly cleaned and numbed with anaesthetic drops to ensure comfort. A very fine needle is then used to deliver the medication into the vitreous the gel-like substance inside the eye allowing the drug to reach the back of the eye quickly.
The entire process usually takes only a few minutes. Most patients feel little more than mild pressure, and recovery is typically quick, with normal activities resumed shortly after. As wet AMD is a long-term condition, injections are often given on a regular schedule basis and adjusted based on how the eye responds during follow-up visits.
Benefits of intravitreal injections include:
- Slowing or stopping further loss of central vision in wet AMD
- Reducing fluid leakage and swelling in the retina
- Helping preserve daily visual function such as reading and recognising faces
- Improving vision in some patients, especially when treatment begins early
- Allowing ongoing monitoring and adjustment of treatment for long-term vision protection
Recovery & Aftercare after Intravitreal Injections
After an intravitreal injection, most patients recover quickly and can return to normal activities within a short time. Some mild discomfort, redness, or temporary visual changes are common and usually settle on their own. Following the recommended aftercare helps reduce the risk of infection, supports proper healing, and ensures the best possible treatment outcome.
Intravitreal Injections Treatments Aftercare
Use this timeline as a quick guide to know what to do & what to avoid, as your eyes heal.
Avoid rubbing or pressing on the eye.
Avoid getting water directly into the eye (no splashing).
Avoid dusty environments if possible.
Avoid eye make-up after the injection.
Resume driving or work once your vision feels stable.
Light exercise is generally safe, avoid rubbing the eye.
Save to travel or fly, follow doctor's advice.
Avoid swimming and hot tubs.
About Dr Errol Chan
Dr Errol Chan is the Medical Director and Senior Consultant Ophthalmologist at Ascend Eye Clinic Singapore, with a subspecialty focus on medical and surgical retinal diseases, including age-related macular degeneration (AMD).
With more than 18 years of clinical and surgical experience and over 10,000 eye procedures performed, Dr Chan provides comprehensive and individualised care for patients with routine and complex retinal diseases, from early diagnosis to long-term management.
Dr Chan obtained his medical degree (MBBS) with Distinction from the National University of Singapore and completed his ophthalmology specialist training at the National University Hospital, Singapore. He holds Ophthalmology specialist accreditations from the Royal Colleges in Edinburgh, Glasgow, London and Canada, as well as the Academy of Medicine, Singapore.
Dr Chan is an international triple fellowship-trained specialist in retinal diseases and retinal surgery. He was awarded a scholarship by the Retina Foundation of Canada to pursue a Vitreoretinal Surgery Fellowship at McGill University, Canada, and has also completed Advanced Vitreoretinal Surgery and Medical Retina & Uveitis Fellowships at the world-renowned Moorfields Eye Hospital London, UK.
In the management of dry and wet age-related macular degeneration, Dr Chan holds expertise in advanced imaging, intravitreal injections, photodynamic therapy, and surgery for complex and treatment-resistant disease. His management approach emphasises early detection, evidence-based treatment, clinical expertise and forefront technology to improve vision and support long-term retinal health.
As a retinal specialist, Dr Chan also manages various medical and surgical retinal diseases, such as diabetic eye disease, retinal detachment, macular hole, epiretinal membrane, retinal vascular and choroidal diseases, uveitis and inherited retinal diseases. He is consulted frequently for second opinions on complex retinal cases, including those for Indonesian patients.
Dr Chan has authored more than 40 peer-reviewed journal publications and textbook chapters, presented at international Ophthalmology conferences, and participated as an investigator in international clinical trials advancing treatments for retinal disease. His work has been recognised with multiple international awards, including accolades from the Asia-Pacific Vitreoretinal Society.

Frequently Asked Questions (FAQs)
1. Will the injection hurt?
The injection will not hurt. There may be slight pressure experienced, but no pain. The eye is numbed with anaesthetic medications before the procedure to fully optimise the comfort of the procedure.
2. How many injections will I need for wet AMD?
Wet AMD is a life-long condition and many patients require ongoing injections. The interval between injections can now be shortened with the use of newer anti-VEGF medications, which have a much longer duration of action. We offer the full range of anti-VEGF medications, so that patients can have an individualised approach that minimally inconveniences them in terms of repeated treatment visits.
3. Can my vision improve after treatment?
Yes. Treatment with anti-VEGF medications reduces fluid leakage, bleeding and scarring in the retina and preserves vision. When treatment is started early, vision can be significantly improved. In more advanced stages of wet AMD, treatment is effective in stabilising vision and preventing further vision loss.
4. How soon should treatment start after diagnosis?
Treatment should begin as soon as possible, particularly for wet AMD, to reduce the risk of rapid central vision loss.
5. What happens if treatment is delayed?
Delaying treatment can lead to further damage to the macula and reduced chances of preserving central vision.
6. How long do I need to stay in Singapore for AMD treatment?
Many patients only need a short stay for consultation and the first injection. Follow up plans can often be coordinated around travel.
7. Can I fly back to Indonesia after intravitreal injections?
Yes. Most patients can travel shortly after injections. Your doctor will advise based on eye condition and response.
8. Will I need treatment for life?
Some patients need long term treatment, while others may require fewer injections over time. This depends on disease activity.
9. Will treatment affect my daily activities?
Most patients resume normal activities within a short time. Temporary redness or mild discomfort may occur.
10. Is Bahasa Indonesia support available for treatment in Singapore?
Yes. Bahasa Indonesia support is available to assist with appointments, communication, and coordination of care.
To learn more or schedule your consultation, contact our Indonesia office via WhatsApp. We’re here to help you.




